Preservation First® is Dr. DiFelice’s unique approach to surgery, based on the belief and confidence in the human body to heal itself. This approach chooses the least invasive surgical option, which favors repairs over replacements, and replacing as little as possible when a repair can’t be done. Dr. DiFelice’s goal for each patient is the smallest surgery for the best outcome possible. Thousands of orthopedic surgeries later, Dr. DiFelice’s philosophy is reinforced time and time again as patients recover their strength and mobility with limited downtime following their procedure.
Background
While studying at some of the best medical institutions in the world, Dr. DiFelice found himself questioning the surgical approaches he was being taught. “If a patient has this injury, then you do this surgery,” seemed to be the shared thought among the medical community. While tried-and-true, this approach was based on research and experience of decades prior, and on decades-old technology as well. Times change, and new technologies evolve that can provide doctors with options that had never existed before. While the one-size-fits-all approach was convenient for doctors at the time, Dr. DiFelice found it to be increasingly far less so for patients.
For his first 5 years in practice, he did as he was taught – and was frustrated by the outcomes. Patients who had more resources had better outcomes than those who had less, which is what we now know as health disparities. These social determinants of healthcare played too pivotal a role in a patient’s postoperative outcome, and Dr. DiFelice had the sense there had to be a better way, one that focused on the healing potential of the human body and was customized to the particular problem of the patient. In other words, not every patient needed the same surgery. Following this discovery, Preservation First® was born, and Dr. DiFelice has been practicing and expanding on his Preservation First® approach for the last 12 years.
Preservation First® Procedures
When it comes to surgery, less is more. In an ideal world, an injury can be treated without surgery, and the body can be allowed to heal on its own. When surgery is necessary, the Preservation First® approach prefers a small operation to anatomically arrange the tissue or other structures and give the body the chance to heal, rather than a bigger operation to replace the entire thing. The solution to injury is not always all or none. Using this approach, the body is left to heal, rather than forced to heal.
Rather than offer every patient the same procedure, Dr. DiFelice provides them with a spectrum of small, medium, and larger surgical options, depending on the injury or condition. The Preservation First® approach to surgery can be applied to all parts of the body, including the knee, shoulder, hip, and more.
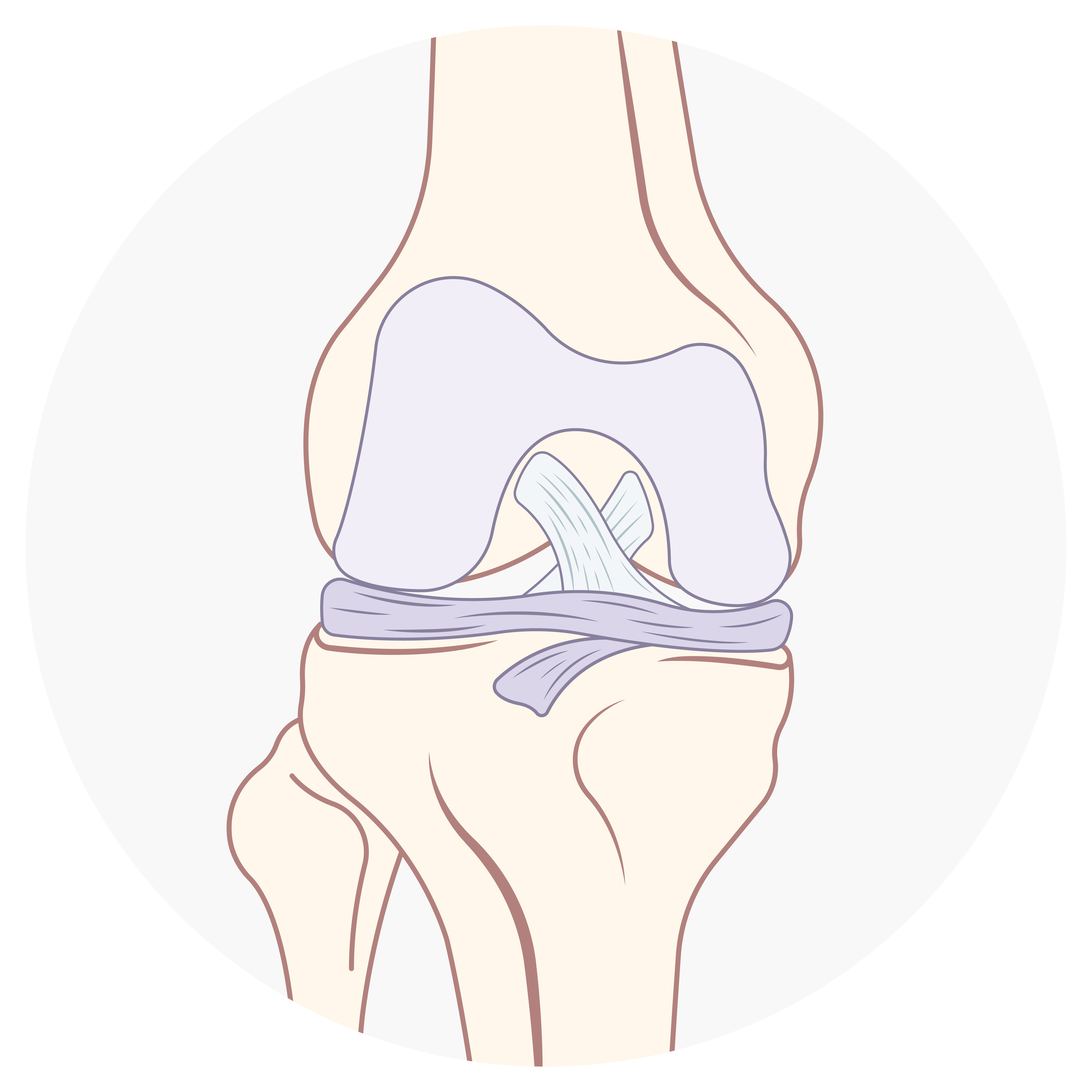
HEALTHY ACL
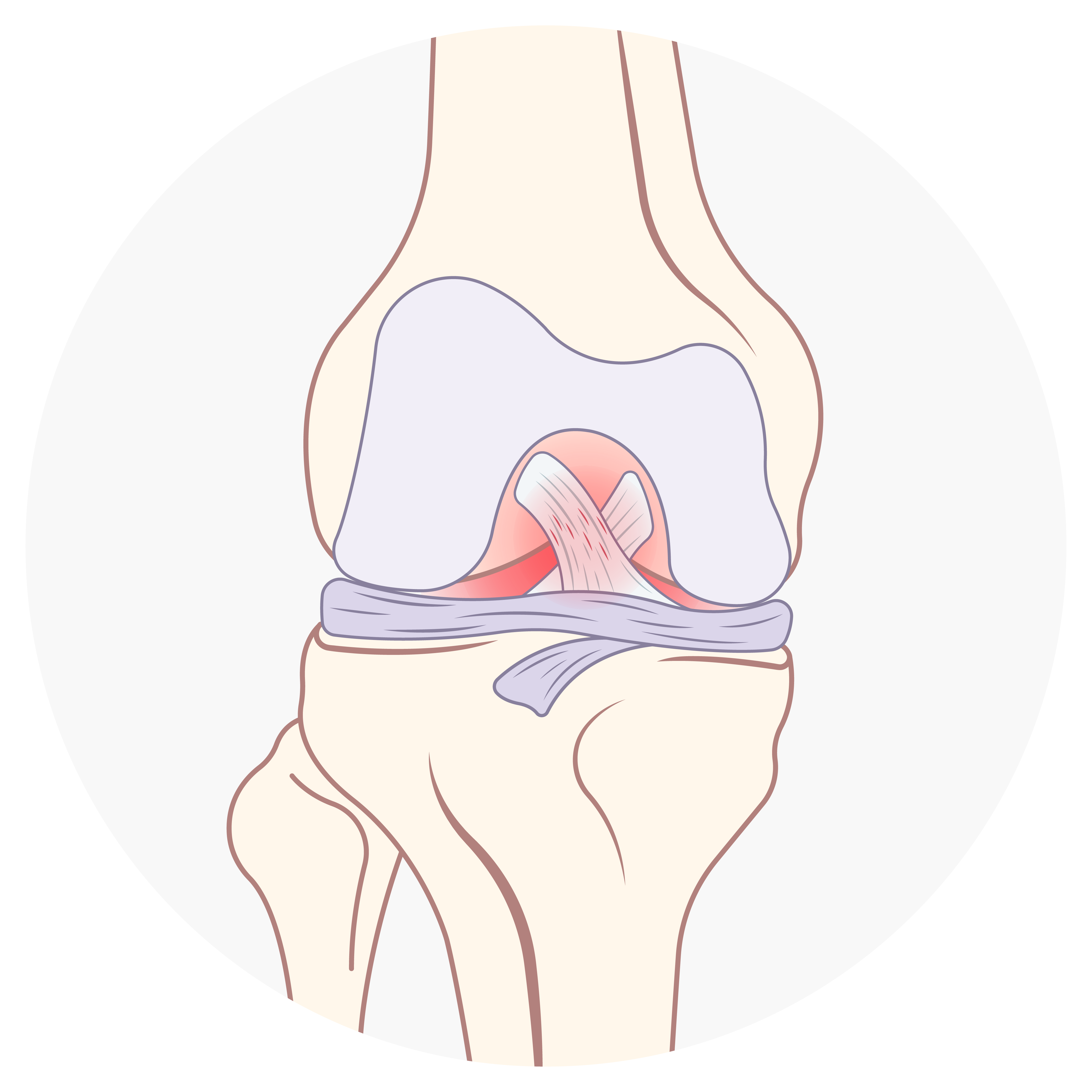
MILD INJURY
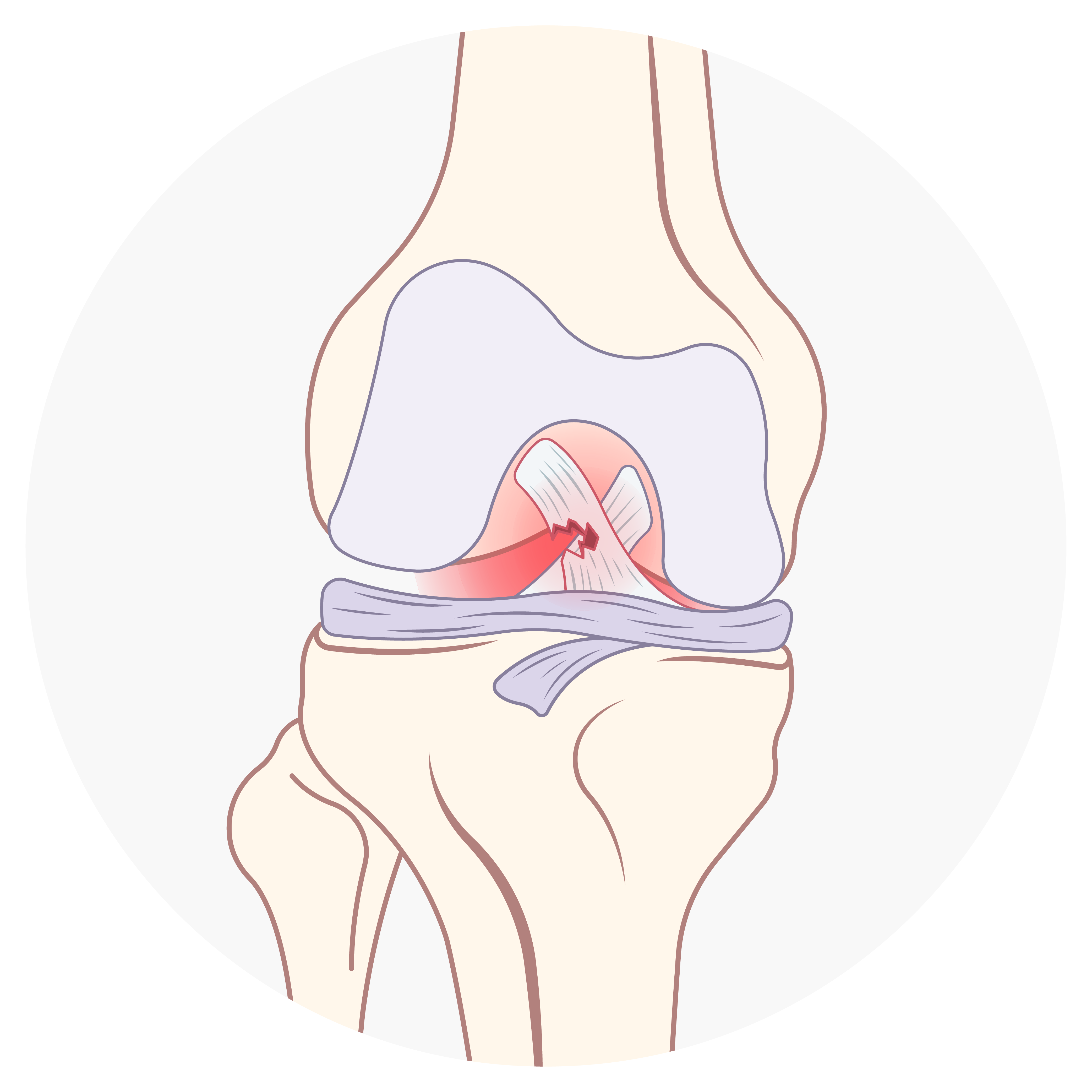
PARTIAL TEAR
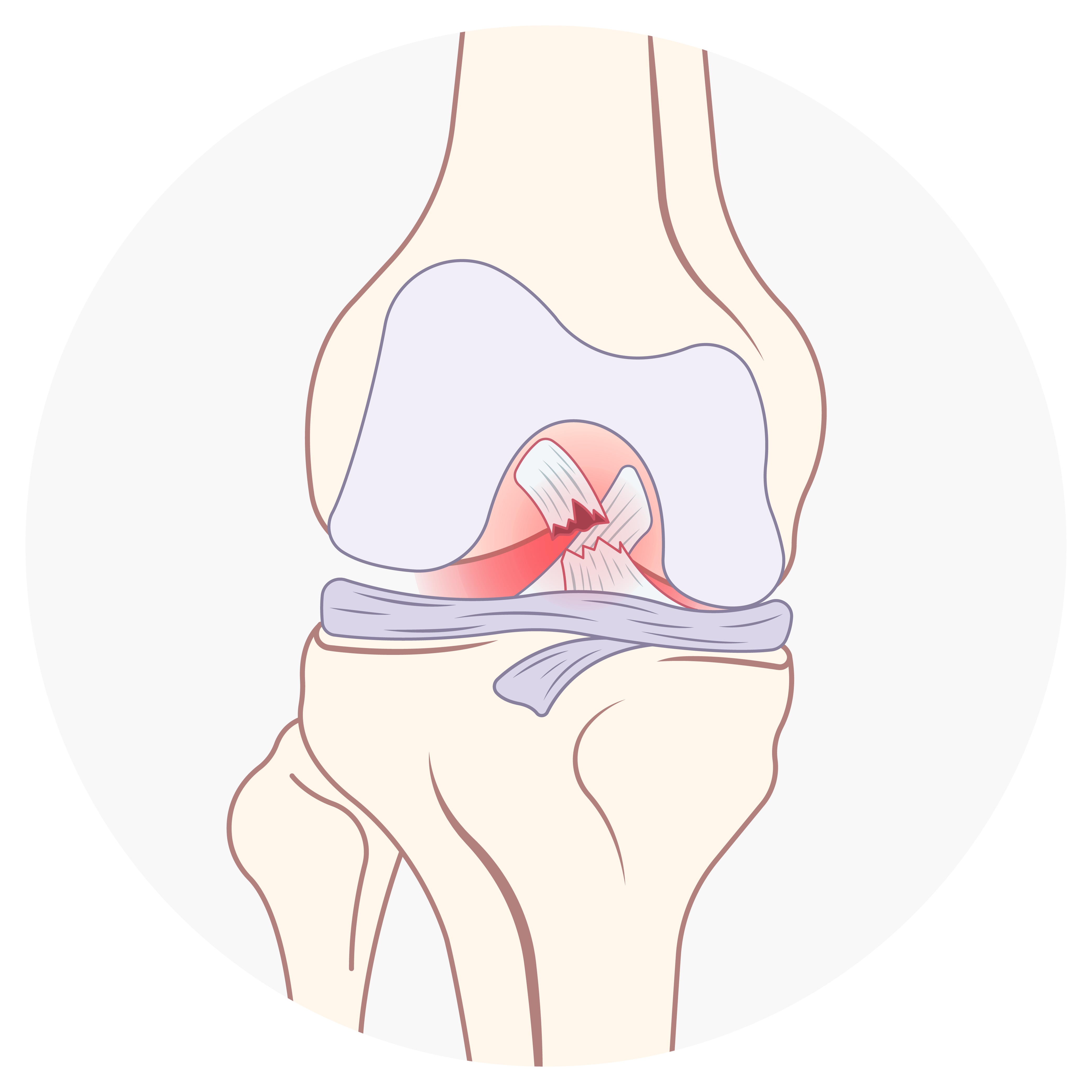
COMPLETE TEAR
A perfect example of the Preservation First® approach is with ACL repairs. When a patient has a torn ACL, it’s common practice for orthopedic surgeons to reconstruct the ACL tendon using a graft from the patient or a deceased donor. However, understanding that not all ACL tears are the same, Dr. DiFelice identifies certain situations where the patient’s tendon can undergo an ACL repair instead of a reconstruction – a much less-invasive procedure that has a recovery time of 4-6 weeks instead of 4-5 months.
Preservation First® Recovery
Surgery is technically a controlled injury to the body, and as with any injury, there will be bleeding, swelling, and discomfort that can lead to stiffness and disability. While using the Preservation First® approach minimizes these potential problems, as well as the need for narcotic pain medications, there is still work to be done by the patient following the procedure. It is critical after surgery to immediately begin working on all of these things so as to minimize their damaging effects and achieve optimal outcomes. Dr. DiFelice is a firm believer in the importance of physical therapy in rehabilitation, and his patients will most likely begin a physical therapy program immediately following surgery to avoid the side effects of immobilization.
We use a team-based approach to treatment and recovery, providing patients with multiple points of contact as they progress through surgery and rehabilitation. Providing education is key, so patients can fully understand what is going to be done during surgery and so they can be the most important part of the team when it comes to recovery. Knowledge is power, and the understanding of the surgical and rehabilitative experience is critical to a great outcome.
Learn More on Preservation First®
Dr. DiFelice has dedicated much of his career research to ligament preservation and developing the Preservation First® approach. To date, he and his team have published over 30 peer-reviewed articles and 5 book chapters on topics related to ACL preservation and/or general ligament preservation. A list of articles and additional research can be found under “Meet Dr. DiFelice”.

