Understanding A Knee Injury
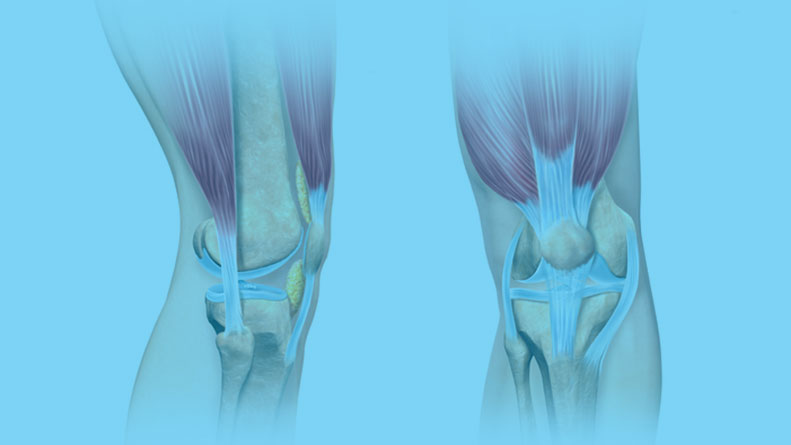
Knee Anatomy
The knee is a complex joint made up of different structures including bones, tendons, ligaments, and muscles. They all work together to maintain normal function and provide stability to the knee during movement.
Having a well-functioning healthy knee is essential for our mobility and ability to participate in various activities. Understanding the anatomy of the knee enhances your ability to discuss and choose the right treatment procedure for knee problems with your doctor.
Ligaments
Muscles
Tendons
Articular Cartilage & Menisci
Bones
Ligaments
Ligaments of the Knee
Ligaments are tough bands of tissue that connect one bone to another bone. The ligaments of the knee function to stabilize the knee joint. There are two important groups of ligaments that hold the bones of the knee joint together, collateral ligaments and the cruciate ligament.
Collateral ligaments are present on either side of the knee. They function to prevent the knee from moving too far during side to side motion. The collateral ligament on the inside is called the medial collateral ligament (MCL) and the collateral ligament on the outside is called the lateral collateral ligament (LCL).
Cruciate ligaments, present inside the knee joint, control the back-and-forth motion of the knee. The cruciate ligament in the front of the knee is called the anterior cruciate ligament or ACL and the cruciate ligament in the back of the knee is called the posterior cruciate ligament or PCL.
Muscles
Muscles of the Knee
There are two major muscles, the quadriceps and the hamstrings, which enable movement of the knee joint. The quadriceps muscles are in the front of the thigh. When the quadriceps muscles contract, the knee straightens. The hamstrings are in the back of the thigh. When the hamstring muscles contract, the knee bends.
Tendons
Tendons of the Knee
Tendons are structures that attach muscles to the bone. The quadriceps muscles of the knee meet just above the patella and attach to it through a tendon called the quadriceps tendon. The patella further attaches to the tibia through a tendon called the patella tendon. The quadriceps muscle, quadriceps tendon, and patellar tendon all work together to straighten the knee. Similarly, the hamstring muscles at the back of the leg are attached to the knee joint with the hamstring tendon.
Articular Cartilage & Menisci
Articular Cartilage and Menisci of the Knee
Movement of the bones causes friction between the articulating surfaces. To reduce this friction, all articulating surfaces involved in movement are covered with a white, shiny, slippery layer called articular cartilage. The articulating surface of the femoral condyles, tibial plateaus, and the back of the patella are covered with this cartilage. The cartilage provides a smooth surface that facilitates easy movement.
To further reduce friction between the articulating surfaces of the bones, the knee joint is lined by a synovial membrane which produces a thick, clear fluid called synovial fluid. This fluid lubricates and nourishes the cartilage and bones inside the joint capsule.
Within the knee joint, between the femur and tibia, there are two C shaped cartilaginous structures called menisci. Menisci function to provide stability to the knee by spreading the weight of the upper body across the whole surface of the tibial plateau. The menisci help in load- bearing by preventing the weight from concentrating onto a small area, which could damage the articular cartilage. The menisci also act as a cushion between the femur and tibia by absorbing the shock produced by activities such as walking, running, and jumping.
Bones
Bones of the Knee
The knee is a hinge joint made up of two bones, the thighbone (femur) and the shinbone (tibia). There are two round knobs at the end of the femur called femoral condyles which articulate with the flat surface of the tibia called the tibial plateau. The tibia plateau on the inside of the leg is called the medial tibial plateau, and on the outside of the leg it is called the lateral tibial plateau.
The two femoral condyles form a groove on the front (anterior) side of the knee called the patellofemoral groove. A small bone called the patella sits in this groove and forms the kneecap. It acts as a shield and protects the knee joint from direct trauma.
A fourth bone called the fibula is the other bone of the lower leg. This forms a small joint with the tibia. This joint has very little movement and is not considered a part of the main joint of the knee.
Conditions
Knee Pain
ACL Tears
LCL Tears
MCL Tears
PCL Tears
Multiligament Tears
Meniscal Tears
Osteoarthritis
Knee Pain
What is Knee Pain?
Knee pain is a common condition affecting individuals from different age groups. It not only affects movement but also impacts the quality of life of the individual. An injury or disease of the knee joint or any structure surrounding the knee can result in knee pain. A precise diagnosis of the underlying cause is important to develop an appropriate treatment plan. Dr. Gregory DiFelice specializes in diagnosing and treating knee pain.
Causes of Knee Pain
Some of the common causes for knee pain include:
- Arthritis: a condition associated with inflammation of the joint
- Knee ligament injuries
- Torn meniscus
- Patellar tendonitis: inflammation of the patellar tendon which connects the kneecap to the shinbone
- Chondromalacia patellae: softening of the articular cartilage on the under surface of the kneecap causing knee pain
- Dislocated kneecap
- Baker’s cyst: a fluid-filled swelling in the back of the knee which usually results from another problem such as a meniscus tear
- Knee bursitis: inflammation of the bursae, small fluid-filled sacs located around the joints, usually between a tendon and the bone.
- Plica syndrome: results from inflammation of the synovial tissue of the knee causing knee pain and swelling.
- Osgood-Schlatter disease: caused by irritation of the growth plate at the front of the knee joint and is more common in adolescents
- Osteochondritis dissecans: characterized by detachment of a cartilage fragment and a thin layer of the bone from the end of a bone due to inadequate blood supply; these fragments may either stay in place or slide around the joint causing pain and joint instability
- Gout: characterized by sudden, severe attacks of joint pain, with swelling and redness around the joint, caused by accumulation of uric acid crystals in the joints
Diagnosis of Knee Pain
Knee conditions should be evaluated by your doctor for a proper diagnosis and treatment. A detailed medical history and physical examination of the knee are crucial for the diagnosis. Your doctor may also conduct diagnostic imaging studies such as X-rays, MRI scans, CT scans, and ultrasound. Blood tests may be performed to identify any infection, gout or pseudogout. Sometimes, arthrocentesis may also be performed, wherein the fluid from the knee joint is removed and sent for laboratory analysis.
Treatment of Knee Pain
Treatment options depend upon the underlying cause responsible for knee pain. Some of the common treatment options for knee pain include rest, ice and heat application, non-steroidal anti-inflammatory medications, stretching, physical therapy and cortisone injections.
Sometimes, a knee arthroscopy may be performed. Knee arthroscopy is a surgical procedure in which the internal structures of the joint are examined to diagnose as well as treat the underlying problem.
If you have trouble or inability to walk, deformity around the joint, inability to bend the knee, knee pain persisting beyond a few days and more at night, or pain associated with swelling, warmth, or redness, you should consult Dr. Gregory DiFelice for immediate medical intervention.
For more information, please contact our office to schedule you appointment today.
ACL Tears
What is an Anterior Cruciate Ligament (ACL) Tear?
The anterior cruciate ligament, or ACL, is one of the major ligaments of the knee that is in the middle of the knee and runs from the femur (thighbone) to the tibia (shinbone). It prevents the tibia from sliding out in front of the femur. Together with the posterior cruciate ligament (PCL), it provides rotational stability to the knee. Overloading this ligament can result in tearing of the ligament fibers, resulting in instability. Dr. Gregory DiFelice specializes in diagnosing and treating ACL injuries.
Causes of ACL Tears
An ACL injury is a sports-related injury that occurs when the knee is forcefully twisted or hyperextended. An ACL tear usually occurs with an abrupt directional change with the foot fixed on the ground or when the deceleration force crosses the knee. Changing direction rapidly, stopping suddenly, slowing down while running, landing from a jump incorrectly, and direct contact or collision, such as a football tackle can also cause injury to the ACL.
Symptoms of ACL Tears
When you injure your ACL, you might hear a “popping” sound and you may feel as though the knee has given way. Within the first two hours after injury, your knee will swell, and you may have a buckling sensation in the knee during twisting movements.
Diagnosis of ACL Tears
To diagnose an ACL injury, Dr. Gregory DiFelice will perform a thorough physical examination of the knee and order additional diagnostic tests, such MRI scans. X-rays may be necessary to rule out any fractures.
Additionally, Dr. Gregory DiFelice will often perform the Lachman’s test to see if the ACL is intact. During a Lachman test, a knee with a torn ACL may show an increased forward movement of the tibia and a soft or mushy endpoint.
A pivot shift test is another method to assess ACL tear. During the pivot shift test, Dr. Gregory DiFelice will rotate your shin while bending your knee. A knee with a torn ACL will cause a “clunking” sensation.
Treatment of ACL Tears
Treatment options include both non-surgical and surgical methods. If the overall stability of the knee is intact, your doctor may recommend non-surgical methods. Non-surgical treatment consists of rest, ice, compression, and elevation (RICE protocol); all assist in controlling pain and swelling. Physical therapy may be recommended to improve knee motion and strength. A knee brace may be needed to help immobilize your knee.
Athletes will most likely require surgery to safely return to sports. Dr. DiFelice has pioneered the Preservation First™ approach to treating ACL injuries. You may learn more by clicking here.
For more information, please contact our office to schedule your appointment today.
LCL Tears
What is a Lateral Cruciate Ligament (LCL) Tear?
The lateral collateral ligament (LCL), also known as the fibular collateral ligament (FCL), is one of four major ligaments of the knee, is situated on the outer part of your knee. It connects the thighbone (femur) to the shinbone (tibia). The LCL limits side-to-side motion of the shinbone. Overloading this ligament can result in tearing of the ligament fibers, resulting in instability. Dr. Gregory DiFelice specializes in diagnosing and treating LCL injuries.
Causes of LCL Tears
Isolated LCL injuries are relatively uncommon, however can occur by direct contact to the inside portion of your knee. More commonly, the LCL is injured along with the lateral meniscus, the anterior or posterior cruciate ligaments, or the posterolateral corner of the knee. These injuries often require high energy, such as collision injuries in football.
Injuries to the LCL can be graded as I, II, or III depending on the severity of injury.
- In grade I, the ligament is mildly damaged and slightly stretched, but the knee joint is stable.
- In grade II, there is partial tear of the ligament.
- In grade III, there is complete tear of the ligament and the ligament is divided into two halves making the knee joint unstable.
Symptoms of LCL Tears
Patients with an LCL tear have symptoms such as knee pain, swelling, and locking or catching sensation in the knee during movement. Patients may also feel as though their knee may ‘give way’’ suddenly or buckle. Pain is commonly located along the outer side of the knee.
Diagnosis of LCL Tears
Dr. Gregory DiFelice will diagnose an LCL injury based on a physical examination of your knee. To determine looseness of the ligament, a varus stress test will be performed by exerting pressure on the inside of your knee while your knee is bent to 30 degrees and then when your knee is completely straight. In addition, other tests such as knee joint X-rays and MRI scans may be done.
Treatment of LCL Tears
Treatment options may include non-surgical and surgical treatment. Non-surgical treatment consists of rest, ice, compression, and elevation (RICE protocol); all assist in controlling pain and swelling. Physical therapy may be recommended to improve knee motion and strength. A knee brace may be needed to help immobilize your knee. Crutches may be recommended to protect your knee.
Generally, surgery is considered in patients with grade III, or complete, tears. Using his Preservation First™ approach, Dr. Gregory DiFelice will assess if you will need a repair or reconstruction of your LCL. This will be based off of your age, injury, tissue quality, and tear pattern. Repairing your ligament will involve stitching the torn sections of the ligament back to the bone, then anchoring a sturdy stitch, called an internal brace, from your femur (thigh bone) to your tibia (shin bone). If the tissue quality is poor, Dr. Gregory DiFelice may need to reconstruct the ligament using a tissue graft which is taken from another part of your body, or a cadaver (another human donor). Following LCL repair or reconstruction, a rehabilitation program will be started that helps you resume a wider range of activities. Usually, a complete recovery may take about 9 to 12 months depending on your injury pattern.
For more information, please contact our office to schedule your appointment today.
MCL Tears
What is a Medial Collateral Ligament (MCL) Tear?
The medial collateral ligament (MCL) is an hour-glassed shaped ligament that is located on the inner part of the knee joint. It runs from the femur (thighbone) to the top of the tibia (shinbone) and helps in stabilizing the knee. The MCL limits side-to-side motion of the shinbone. This ligament helps stabilize the knee. Overloading this ligament can result in tearing of the ligament fibers, resulting in instability. Dr. Gregory DiFelice specializes in diagnosing and treating MCL injuries.
Causes of MCL Tears
The medial collateral ligament (MCL) injuries commonly occur in contact, collision, and twisting sports, such as football, tennis, and skiing. The MCL may be injured with direct contact to the outside portion of your knee. Noncontact injuries may occur when your shoe catches on a playing surfaces, such as turf, while quickly trying to change direction.
Injuries to the MCL can be graded as I, II, or III depending on the severity of injury.
- In grade I, the ligament is mildly damaged and slightly stretched, but the knee joint is stable.
- In grade II, there is partial tear of the ligament.
- In grade III, there is complete tear of the ligament and the ligament is divided into two halves making the knee joint unstable.
Symptoms of MCL Tears
Patients with an MCL tear have symptoms such as knee pain, swelling, and locking or catching sensation in the knee during movement. Patients may also feel as though their knee may ‘give way’ suddenly or buckle. Pain is commonly located along the inner side of the knee.
Diagnosis of MCL Tears
Dr. Gregory DiFelice will diagnose an MCL injury based on a physical examination of your knee. To determine looseness of the ligament, a valgus stress test will be performed by exerting pressure on the outside of your knee while your knee is bent to 30 degrees and then when your knee is completely straight. In addition, other tests such as knee joint X-rays and MRI scans may be done.
Treatment of MCL Tears
Treatment options include non-surgical and surgical treatment. Non-surgical treatment consists of rest, ice, compression, and elevation (RICE protocol); all assist in controlling pain and swelling. A knee brace may be worn to help immobilize your knee. Use of crutches may be recommended to protect your knee. Physical therapy exercises may be recommended to improve knee motion and strength. The healing time for non-surgical MCL injuries is typically between 2-6 weeks depending on the injury pattern.
Generally, surgery is considered in patients with grade III, or complete, tears. Using his Preservation First™ approach, Dr. Gregory DiFelice will assess if you will need a repair or reconstruction of your MCL. This will be based off of your age, injury, tissue quality, and tear pattern. Repairing your ligament will involve stitching the torn sections of the ligament back to the bone, then anchoring a sturdy stitch, called an internal brace, from your femur (thigh bone) to your tibia (shin bone). If the tissue quality is poor, Dr. Gregory DiFelice may need to reconstruct the ligament using a tissue graft which is taken from another part of your body, or a cadaver (another human donor). Following MCL repair or reconstruction, a rehabilitation program will be started that helps you resume a wider range of activities. Usually, a complete recovery may take about 6 to 12 months depending on your injury pattern.
For more information, please contact our office to schedule your appointment today.
PCL Tears
What are Posterior Cruciate Ligament (PCL) Tears?
The posterior cruciate ligament (PCL), one of four major ligaments of the knee, is situated at the back of the knee. It connects the thighbone (femur) to the shinbone (tibia). The PCL limits the backward motion of the shinbone. Overloading this ligament can result in tearing of the ligament fibers, resulting in instability. Dr. Gregory DiFelice specializes in diagnosing and treating PCL injuries.
Causes of PCL Injuries
The PCL is usually injured by a direct impact, such as in an automobile accident when the bent knee forcefully strikes the dashboard. In sports, it can occur when an athlete falls to the ground with a bent knee or through direct contact. A majority of PCL injuries occur in combination with other injuries with the knee, consistent with multi-ligament trauma. Twisting injury or overextending the knee can cause the PCL to tear. PCL injuries are very rare and are more difficult to detect than other knee ligament injuries. Cartilage injuries, bone bruises, and ligament injuries often occur in combination with PCL injuries.
Injuries to the PCL can be graded as I, II, or III depending on the severity of injury.
- In grade I, the ligament is mildly damaged and slightly stretched, but the knee joint is stable.
- In grade II, there is partial tear of the ligament.
- In grade III, there is complete tear of the ligament and the ligament is divided into two halves making the knee joint unstable.
Symptoms of PCL Injuries
Patients with PCL injuries usually experience knee pain and swelling immediately after the injury. There may also be instability in the knee joint, knee stiffness that causes limping, and difficulty in walking.
Diagnosis of PCL Injuries
Diagnosis of a PCL tear is made based on your symptoms, medical history, and by performing a physical examination of the knee. Other diagnostic tests such as X-rays and MRI scans may be ordered. X-rays are useful to rule out avulsion fractures wherein the PCL tears off a piece of bone along with it. An MRI scan is done to help view the images of soft tissues better. Dr. Gregory DiFelice will perform a posterior drawer test. During this test, a knee with a torn PCL may show an increased backward movement of the tibia and a soft or mushy endpoint.
Treatment of PCL Injuries
Treatment options may include non-surgical and surgical treatment. Non-surgical treatment consists of rest, ice, compression, and elevation (RICE protocol); all assist in controlling pain and swelling. Physical therapy may be recommended to improve knee motion and strength. A knee brace may be needed to help immobilize your knee. Crutches may be recommended to protect your knee.
Generally, surgery is considered in patients with knee dislocations or complete tears. Surgery is performed arthroscopically with a few small incisions. Using his Preservation First™ approach, Dr. Gregory DiFelice will assess if you will need a repair or reconstruction of your PCL. This will be based off of your age, injury, tissue quality, and tear pattern. Repairing your ligament will involve stitching the ligament back to your femur (thigh bone) with absorbable anchors. If the tissue quality is poor, Dr. Gregory DiFelice may need to reconstruct the ligament using a tissue graft which is taken from another part of your body, or a cadaver (another human donor). Following PCL repair or reconstruction, a rehabilitation program will be started that helps you resume a wider range of activities. Usually, a complete recovery may take about 9 to 12 months depending on your injury pattern.
For more information, please contact our office to schedule your appointment today.
Multiligament Tears
What are Multiligament Tears?
The knee is a complex joint of the body which is vital for movement. The four major ligaments of the knee are the anterior cruciate ligament, posterior cruciate ligament, medial collateral ligament, and lateral collateral ligament. They play an important role in maintaining the stability of the knee. An injury resulting in tear of one or more ligaments of the knee thus affects knee stability. Dr. Gregory DiFelice specializes in diagnosing and treating multiligament injuries.
Causes of Multiligament Tears
Multiligament tears are often from high energy injuries. These could include a direct blow to the knee, or a fall from a height, or motor vehicle trauma. Multiligament knee injuries are common in athletes involved in contact sports such as soccer, football, and basketball, or non-contact sports, like skiing.
Symptoms of Multiligament Tears
Such injuries occurs because of a direct blow to the knee, or a fall from a height, or motor vehicle trauma. Multiple ligament knee injuries are common in athletes involved in contact sports such as soccer, football, and basketball. Patients with multi-ligament knee injuries may experience pain, swelling, limited range of motion, injuries to nerves and arteries of the leg, and knee instability.
Diagnosis of Multiligament Tears
Sometimes, knee pain due to other injuries results in involuntary movements that give the sensation of instability. A thorough examination by Dr. Gregory DiFelice is very crucial for the correct diagnosis of multiligament instability. Other diagnostic tests such as X-rays and MRI scans may be ordered. X-rays are useful to rule out fractures, while an MRI scan can help better visualize the soft tissues.
Treatment of Multiligament Tears
Usually grade I (mild tear) and grade II (partial tear) multiligament injuries are treated conservatively with rest, ice, compression, and elevation. But, treatment of grade III (complete tear) multiligament injuries requires surgery.
Generally, surgery is considered in patients with knee dislocations or complete tears. Surgery is performed both arthroscopically and open, based off of your injury patterns, however, with as incisions as possible. Using his Preservation First™ approach, Dr. Gregory DiFelice will assess if you will need a repair or reconstruction of your ligaments. This will be based off of your age, injury, tissue quality, and tear pattern. Repairing your ligaments will involve stitching the ligaments back to bone. If the tissue quality is poor, Dr. Gregory DiFelice may need to reconstruct your ligaments using tissue grafts which is taken from another part of your body, or a cadaver (another human donor). Following a multifilament repair or reconstruction, a rehabilitation program will be started that helps you resume a wider range of activities. Usually, a complete recovery may take about 12 months depending on your injury pattern.
For more information, please contact our office to schedule your appointment today.
Meniscal Tears
What is a Meniscal Tear?
The two wedge-shaped cartilage pieces present between the thighbone and the shinbone are called meniscus. The meniscus located on the inner side of your knee is called the medial meniscus, while the meniscus located on the outer side of your knee is called the lateral meniscus. They stabilize the knee joint and act as “shock absorbers.” Tears to the meniscus are classified as partial or complex, traumatic or degenerative, and horizontal, vertical, radial, “bucket-handle,” or “parrot-beak.” Dr. Gregory DiFelice specializes in diagnosing and treating meniscal injuries.
Causes of Meniscal Tears
Meniscal tear is the most common knee injury in athletes, especially those involved in contact sports. Meniscal tears typically occur when you quickly change direction, while twisting the knee. This frequently occurs in soccer, basketball, football, and lacrosse. Older patients are more prone to degenerative meniscal tears as the cartilage wears out and weakens with age. This is common in individuals who have some degree of osteoarthritis in their knee.
Symptoms of Meniscal Tears
A torn meniscus causes pain, swelling, stiffness, catching, or a locking sensation in your knee making you unable to move your knee through its complete range of motion.
Diagnosis of Meniscal Tears
Dr. Gregory DiFelice will examine your knee, as well as evaluate your symptoms and medical history before suggesting a treatment plan. Dr. Gregory DiFelice assess for swelling and gauge your range of motion. Additionally, will press along the joint lines of your knee to assess for any pain. Frequently, Dr. Gregory DiFelice will order an MRI to better visualize the meniscus.
Treatment for Meniscal Tears
The treatment depends on the type, size, and location of tear as well your age and activity level. If the tear is small with damage only in the outer edge of the meniscus, non-surgical treatment may be sufficient. However, if the symptoms do not resolve with non-surgical treatment, surgical treatment may be recommended. Non-surgical treatment consists of rest, ice, compression, and elevation (RICE protocol); all assist in controlling pain and swelling. Physical therapy may be recommended to improve knee motion and strength. A knee brace may be needed to help immobilize your knee. Crutches may be recommended to protect your knee.
Generally, surgery is considered in patients with catching or locking symptoms. Surgery is performed arthroscopically with a few small incisions. Using his Preservation First™ approach, Dr. Gregory DiFelice will assess if you will need a meniscal repair or partial meniscectomy. This will be based off of your age, injury, tissue quality, tear pattern, and level of osteoarthritis. Repairing your meniscus will involve stitching the torn sections of the meniscus back together. If the tissue quality is poor, Dr. Gregory DiFelice may need to perform a meniscectomy, which involves removing the torn edges of the meniscus and smoothing out the remaining section. Following meniscal repair or meniscectomy, a rehabilitation program will be started that helps you resume a wider range of activities. Usually, a complete recovery may take about 3 to 6 months depending on your injury pattern.
For more information, please contact our office to schedule your appointment today.
Osteoarthritis
What is Knee Osteoarthritis?
Osteoarthritis is a general term covering numerous conditions where the joint surface or cartilage wears out. The joint surface is covered by a smooth articular surface that allows pain-free movement in the joint. This surface can wear out for several reasons; often the definite cause is not known.
When the articular cartilage wears out, the bone ends rub on one another and cause pain. This condition is referred to as Osteoarthritis or “wear and tear” arthritis, as it occurs with aging and use. It is the most common type of arthritis. Dr. Gregory DiFelice specializes in diagnosing and treating osteoarthritis.
Causes of Knee Osteoarthritis
There are numerous conditions that can cause arthritis but often the exact cause is never known. In general, but not always, it affects people as they get older.
The causes include:
- Trauma, such as fractures or prior knee surgery
- Increased stress such as overuse or prior sports injuries
- Infection of the bone
- Connective tissue disorders
- Inactive lifestyle and being overweight. Your weight is the single most important link between diet and arthritis, as being overweight puts an additional burden on your hips, knees, ankles, and feet.
Symptoms of Knee Osteoarthritis
Knee arthritis causes pain and decreased mobility of the knee joint. Patients often feel stiffness after prolonged sitting, which can eventually loosen up as they begin to walk. Pain can be focal to one part or spread throughout the knee. It is frequent that patients may notice some clicking or “crackling” noises as they walk or go from sitting to standing. Swelling is quite common in osteoarthritis.
Diagnosis of Knee Osteoarthritis
Dr. Gregory DiFelice will examine your knee, as well as evaluate your symptoms and medical history before suggesting a treatment plan. Your initial evaluation will include an x-ray to evaluate the joint spaces in your knee. In the arthritic knee, the space between your femur (thigh bone) and your tibia (shin bone) will be narrower or absent. Additionally, bone spurs or excessive bone can also build up around the edges of the joint. The combinations of these factors make the arthritic knee stiff and limit activities due to pain or fatigue. An MRI scan may be performed to visualize the soft tissues better.
Treatment for Osteoarthritis
The treatment depends on the degree of osteoarthritis, as well as, your age and activity level. If your osteoarthritis is minimal, or in the early stages, non-surgical treatment may be sufficient. Non-surgical treatment consists of rest, ice, compression, and elevation (RICE protocol). Physical therapy may be recommended to improve knee motion and strength. Injection therapy, including corticosteroids and viscosupplementation (hyperlink to injection page), can help patients with early to moderate osteoarthritis. However, if the symptoms do not resolve with non-surgical treatment, surgical treatment may be recommended.
There are several surgical options for knee osteoarthritis. Using his Preservation First™ approach, Dr. Gregory DiFelice will assess if you will need a partial knee replacement or a total knee replacement. Partial knee replacement, or unicompartmental knee replacement, is a robotic assisted knee surgery for patients who have osteoarthritis in one-to-two compartment of their knee. It is performed using robotic-arm technology that allows Dr. Gregory DiFelice to precisely perform the surgery through a smaller incision as compared to traditional surgery. For patients with osteoarthritis located in all three compartments of the knee, Dr. Gregory DiFelice will perform a total knee replacement. This involves replacing the surfaces of your knee with a prosthetic implant. Following partial or total knee replacement, a rehabilitation program will be started that helps you resume a wider range of activities. Usually, a complete recovery may take about 9 to 12 months depending on your level of osteoarthritis.
For more information, please contact our office to schedule your appointment today.

